Must Watch Agrasen Girls PG college- Dr. Anand Srivastava Inaugural lecture
Agrasen Girls PG college- Dr. Anand Srivastava Inaugural lecture-part 2
Agrasen Girls PG college- Dr. Anand Srivastava Inaugural lecture-part 1

Agrasen Girls PG college- Dr. Anand Srivastava Inaugural lecture-part 2
Agrasen Girls PG college- Dr. Anand Srivastava Inaugural lecture-part 1
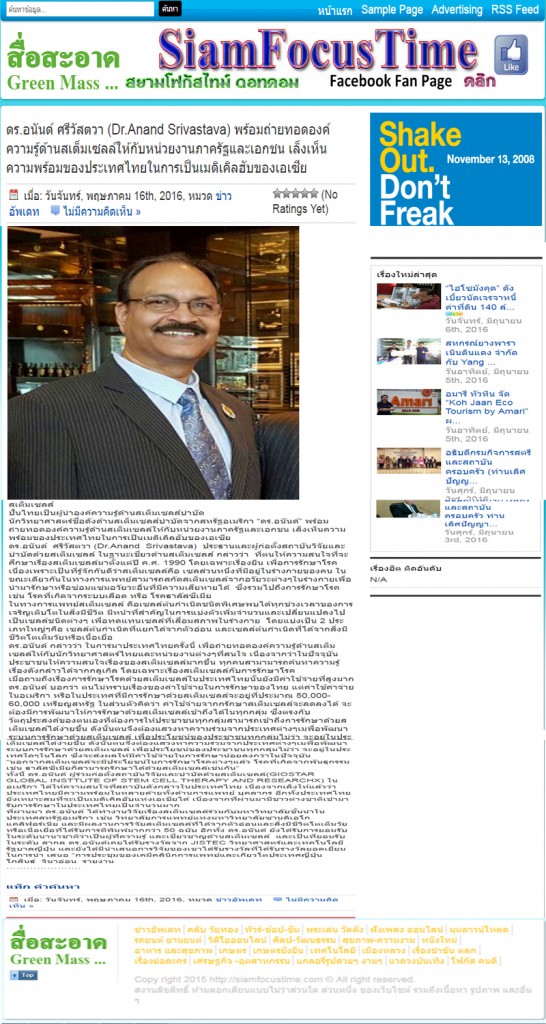
Stem cell plasticity Thailand leading knowledge of stem cell therapy
Scientists celebrated the stem cell therapy in the United States, “Dr. Anand” with knowledge of stem cells for government agencies and. private Sees the availability of a Medical Miracle in the hub of Asia.
Dr. Anand T. Wa Si Sawat (Dr.Anand Srivastava) President and Founder of Research and Therapy, Stem Cells. As a specialist in stem cells, said their attention to studying stem cells since 1990, especially in the genes. For medicinal purposes Because it is well known that stem cells are. The cells are present in a person’s body. Meanwhile, medical extraction of stem cells from different organs in the body in order to maintain or repair other organs are damaged. These include the treatment of diseases such as blood or Roma Katha thalassemia in medical stem cells. Is a special type of stem cells found in all periods of growth in living organisms. An important role in the proliferation of cells proliferate and differentiate into different types. To replace aging cells in the body can be divided into two major categories. Stem cells isolated from embryos. And stem cells derived from adult organisms or tissues Dr. Anand said in Thailand this time. To convey the knowledge of stem cells to scientists and organizations interested Thailand. Because of the current public attention to the issue of stem cells more.
Anyone can find out about the car of the Google logo. In particular, the stem cells to treat disease, when asked about the treatment with stem cells in that the cost is very high, Dr. Anand said he was not aware of the cost of. treatment of ThailandBut the cost in America. Or in countries where the treatment with stem cells is about. 50,000-60,000 US dollars in private thought. The cost of a stem cell treatment can be reduced. It requires the development of a stem cell therapy accessible in all groups. Which meet their objectives requires that all citizens have access to treatment with stem cells more easily. So he had to seek the cooperation of the country’s various family systems therapy with stem cells. For the benefit of all citizens, regardless. In any country in the world. As a result, the cost of maintaining less than the current “In addition, the stem cells would be useful in the treatment of various diseases ago. The disease is caused by genetics, such as thalassemia can be treated with stem cells, “said the Dr. Anand, who co-founded the Institute for Therapy and Stem Cell (GIOSTAR GLOBAL INSTITUTE OF STEM CELL THERAPY AND RESEARCH). America was paying attention to such institutions in the country. The aim, then, that Thailand is ready thread in many of the medical personnel, and also the right to a Medical Miracle hub of Asia. The last foreigners to be treated in a number of past Dr. Anand has done research on stem cells, together with leading universities in the United States, such as the Medical College of the University of San Diego. Diego, CA, with research on embryonic stem cells and adult life. Or tissues that have been published more than 50 editions of The Dr. Anand has also been internationally recognized as the knowledge.And specialized stem cells And is internationally recognized Dr. Anand had won JISTEC of Science and Technology, Government of Japan. And has presented his research won the award for excellence in the presentation of the “Meeting of Clinical Chemistry and Medicine, Kyoto,
Japan,
Mexico Couture Krajina weak report
| The leading Annual Meeting dedicated to the Chemistry Researchers Register today and join over 400 of your Colleagues European Chemistry Congress |
|
|
|
|
Dear Dr. Anand S Srivastava,
“European Chemistry Congress” on June 16-18, 2016 Rome, a leading forum for Chemists, Drug Analysts, Analytical Chemists, Chemical Engineers, New Chemical Technologies Developers, Nuclear Chemists, Experts in Physical Chemistry, Experts in Drug Discovery and Development, Chemical Industry Professionals, Experts in Organic and Inorganic Chemistry, Medical Biochemistry Experts, Computer Aided Drug Design Experts, Pharma Industry Professionals and Scholars in Chemistry related areas and will encourage Innovation, Educate & Invigorate the attendees. European Chemistry Congress is the leading annual meeting dedicated to Chemistry research with the theme of Exploring recent advances in chemistry, related fields and applications and that consistently delivers a cutting-edge agenda, 400+ senior delegates, and a sold-out exhibit hall. |
|
| Program Coverage | |
| Day 1 June 16, 2016 | |
| •Fundamentals of Organic Chemistry •Inorganic Chemistry •Analytical Chemistry •Green Chemistry: Green chemical principles |
|
| Day 2 June 17, 2016 | |
| •Medical Biochemistry •Physical Chemistry •Biological Chemistry •Environmental Chemistry |
|
| Day 3 June 18, 2016 | |
| •Nuclear chemistry •Theoretical Chemistry •Medicinal Chemistry •Multi-disciplinary Chemistry |
|
| 5th European Biosimilars Congress June 27-29, 2016 Valencia, Spain “The European perspective of Biologics and Biosimilars” Meet World leading Biosimilar Industry Leaders from 50+ different Countries |
|
| I hope this message finds you well. I’m honored to request you to speak at 5th European Biosimilars Congress happening from June 27-29, 2016 Valencia, Spain and would be so excited if you would join us. | |
| Euro Biosimilars 2016 is a three day event with an audience from leading industries of Biosimilars and follow-on-Biologics sector, contract research organizations, research institutes, patent attorneys, domestic and international regulatory agencies and executive directors of leading biopharmaceutical companies and experts. | |
| Our goal is to bring together bright minds to give talks that are idea-focused, and on a wide range of subjects, to foster learning, inspiration and wonder – and provoke conversations that matter. | |
| UNIQUE FEATURES OF EURO BIOSIMILARS 2016 | |
| •Our robust on-line publicity attracts 20000+ users and 60000+ views to our Library of Abstracts which brings worldwide exposure to the researchers and speakers participate in our conferences. •The Career Guidance Workshops to the Graduates, Doctorates and Post-Doctoral Fellows •Accepted Abstracts will be published in PubMed, MEDLINE, ProQuest, SCOPUS, SOCOLAR, EBSCO, CAS, Hinari, Index Copernicus, Google Scholar, SCIRUS, DOAJ indexed journals. •Each abstract will be labeled with a Digital Object Identification Number (DOI) provided by Cross Ref •Speaker and Abstract pages created in Google on your name would get worldwide acknowledgment to your research profile |
|
| CONFERENCE TOPICS | |
| • Current Challenges of Biologics • Emerging Biosimilars in Therapeutics • Legal Issues • Regulatory Approach for Biosimilars • Biosimilars Innovator Pharmaceutical Products • Plant Produced Biosimilars • Bioequivalence Assessment |
• Biosimilar Analytical Strategies • Intellectual Property Rights • Globalization of Biosimilars • BCS & IVIVC Based Biowaivers • Biosimilar Market Analysis • Biosimilars Pharmacovigilance • Clinical Studies on Biosimilars • Entrepreneurs Investment Meet |
| Benefits: | |
| •Keynote sessions by world’s most eminent researchers and Networking with Experts in the field of Pharma •Live Streaming of your presentation through our websites and YouTube •e-Poster for $99 •Outstanding Young Researcher Award and Best Poster Award •Top Industries Representation |
|
| For more details visit our website http://biosimilars-biologics.pharmaceuticalconferences.com/europe/ | |
| The Euro Biosimilars 2016 Committee is pleased to announce that they are currently accepting proposals for Symposia and Workshops on the above given topics. All proposals must be submitted to: eurobiosimilars@conferenceseries.com | |
| We believe your voice would be a critical addition to the Euro Biosimilars 2016 stage. Thank you for reading, and we very much look forward to hearing from you. | |
| Best Regards Badoni Victor Program Manager- Euro Biosimilars 2016 Email: biosimilars@conferenceseries.com Contact us America: 2360 Corporate Circle Suite 400 Henderson NV 89074-7722 | USA | Tel: +1-650-268-9744 Europe: Heathrow Stockley Park Lakeside House, 1 Furzeground Way, Heathrow, UB11 1BD, UKAsia-Pacific: 6th Floor | North Block | Divyasree Building | Raidurg | Hyderabad 500032 | Tel: 040-33432300 |
|
| Dear Dr.Anand S Srivastava, |
| OMICS International is pleased to invite you to the 9th World Drug Delivery Summit during June 30-July 02, 2016 at Crowne Plaza New Orleans Airport, New Orleans, USA. |
| We aware of your expertise, tremendous experience and achievements in this field, therefore, we are expecting your presence in the meeting, which will be providing new insights and inspire the young researchers to put forward their ideas and knowledge for the betterment of future generations. |
| Keynote speakers are: |
| Pieter R. Cullis (Director of NanoMedicines Research Group, Canada), Gjumrakch Aliev (President and CEO of GALLY International Biomedical Research, USA), Istvan Toth (Director of Pharmaceuticals TetraQ Group, Australia), Hiroshi Maeda (President Sojo University Institute of Drug Delivery Science Japan), Soumyajit Majumdar, (Associate Dean, University of Mississippi, USA) Sharad Murdane, (Asso. Director, Pfizer Global R&D, USA) Tudor Arvinte, (Chairman, CEO, Therapeomic Inc., Switzerland) |
| For more Details about World Drug Delivery 2016 and Abstract submission, |
|
PS: http://drugdelivery. |
| World Drug Delivery 2016 Highlights: |
| •Drug Delivery Technology •Novel Drug Delivery Systems •Routes of Drug Administration •Pharmaceutical Nanotechnology •Drug Delivery Companies •Nucleic Acid Based Drug Delivery •Smart Drug Delivery Systems •Recent Advances in Drug Delivery •Vaccine Design and Delivery Technology •Drug Delivery and Medical Device Development •Novel Technique in Drug Delivery •Peptide and Protein Drug Delivery •Drug Delivery Equipment and Machinery •Business Opportunities in Drug Delivery |
| Looking Forward to hear from you, to join us in New Orleans |
|
With Best Wishes, Riley Matthews World Drug Delivery 2016 Phone: 1-702-508-5200 Ext: 8046 E-mail: drugdelivery@conferenceseries. |